'I am an NHS doctor using self-care to prevent PTSD'
As Marie Claire launches Women in Tech Week to celebrate the trailblazing women making waves in STEM, we meet Anaesthetist Harriet Wilson to talk symptoms, NHS aftercare and the importance of self-care

Celebrity news, beauty, fashion advice, and fascinating features, delivered straight to your inbox!
You are now subscribed
Your newsletter sign-up was successful
As Marie Claire launches Women in Tech Week to celebrate the trailblazing women making waves in STEM, we meet Anaesthetist Harriet Wilson to talk symptoms, NHS aftercare and the importance of self-care
It's Women in Tech Week at Marie Claire. Marking International Day of Women and Girls in Science on February 11, all this week we'll be sharing stories from the incredible women changing the face of the STEM industries. Next up is 27-year-old NHS anaesthetist Harriet. Faced with the trauma of the pandemic's relentless daily death toll, she's practicing self-care to prevent PTSD.
This is her story.
Article continues below'Working on the frontline during the height of the COVID-19 pandemic could have caused PTSD for any member of NHS staff – it was was completely anxiety-inducing and stressful. Every day was so uncertain and unnerving. I am an Anaesthetic SHO (Senior House Officer), trained to come face to face with death, but coming to terms with the number of people dying every day in-front of me was traumatic. I work in a small district general hospital in London, and normally we have eight beds in intensive care. We went up to 35 in the peak.
Before Covid, I was working on the labour ward, administering epidurals for women going for C-Sections. Suddenly, every anaesthetist in the entire hospital got moved on to an emergency rota of physically and mentally draining 13-hour shifts (compared to 10 hours) and was told to spend the entire shift in intensive care.
My role in ICU was to put patients to sleep and then put a tube down their throat into the airway and attach that tube to the ventilator. Doing something so highly pressured - to get tube into the right place – was made harder by the layers and layers of horribly hot PPE.
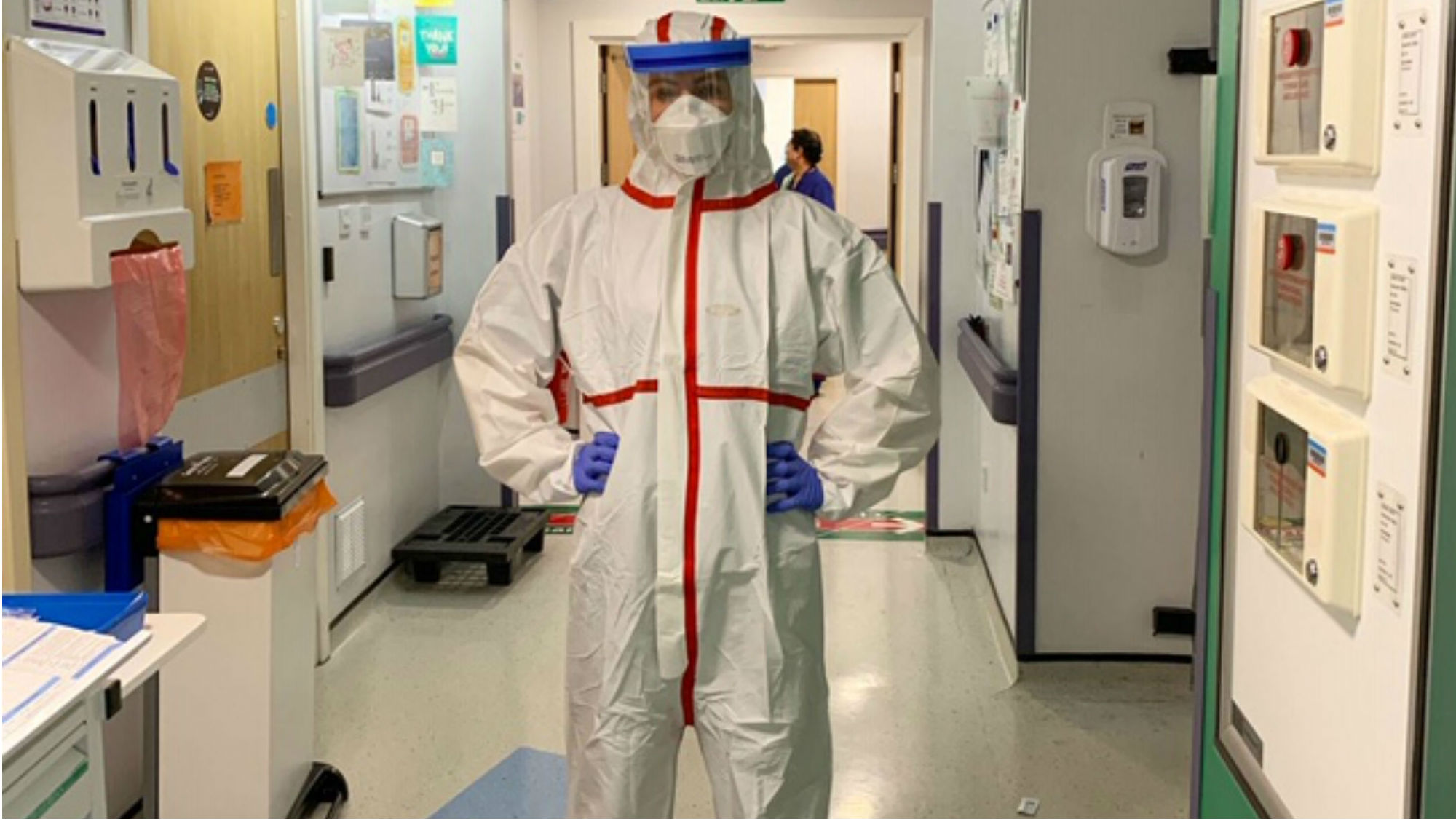
In the past week I have returned to the labour ward on my regular shift pattern. It’s nice to be providing care in other parts of the hospital again and get back to a bit of normality.
Celebrity news, beauty, fashion advice, and fascinating features, delivered straight to your inbox!
Spotting the signs of PTSD
We’ve had two debrief sessions at work, led by one of the female consultants and a clinical psychologist. The aim was to allow us to talk about our feelings following the aftermath of the peak and to learn how to spot the signs of PTSD in colleagues and ourselves. We identified anxiety, nightmares and flashbacks, but the main PTSD symptom we all felt was guilt about not being able to save more people, and both sessions were really useful, but it depended if you were in work and actually free at that time as to whether you could attend one or both sessions. Some colleagues weren’t able to attend either.
I’ve also attended a couple of mindfulness sessions, hosted by one of the midwives. They are only ten minutes long, but popping in really refreshes you to then get back to patients.
Currently, there are no plans for any more debrief sessions to discuss PTSD, but I believe if we asked the consultants they would be happy to hold more. They are aware there is likely to be big implications to our mental health and have shared useful psychological website resources to support us out of hours.
Of course, we anticipated this unknown disease was going to be challenging, but intensive care is scary at the best of times, and with Covid, we were seeing so many die so quickly and unexpectedly. It was shocking to see. I have a huge amount of respect for the junior staff, who provided an invaluable support system to the team. Some were only six months out of university and they truly stepped up in a time of crisis.
Traumatising phone calls
Personally, what traumatised me the most was making phone calls to family members who weren’t allowed to visit, and explaining their loved ones were unlikely to survive the night. When you’re talking face to face, it’s easier to explain and show compassion. Ending every call made me feel sad and quite helpless.
That said, the palliative care team put together beneficial phrases and positioned them next to the phones, and we are going to continue using these in the future to make conversations with family members unable to make it to hospital a little easier.
There have been times when I felt anxious for my health, but I have felt more worried about my family, who live on The Wirral, near Liverpool. My sister is an A&E doctor two years out of university, my dad is a GP and my mum is a nurse. Seeing relatively fit patients of their age come in and become suddenly unwell always made me fear for their wellbeing. I haven’t seen any of them in over three months, which has been tough, but now government rules are relaxed, I’ll drive up and see them in the next few weeks.
Teaching mindfulness
My boyfriend Richard works in intensive care at the same hospital as me, and so at the beginning of the pandemic we decided to isolate together. I’m so grateful to have had someone to debrief the day with, but working all day and talking about Covid all night became a bit all consuming, so we found other ways to release tension – taking part in yoga classes and using the HeadSpace app, which teaches mindfulness and became free for NHS staff to download.

PTSD symptoms do not necessarily present themselves straight away, and that does worry me. You go back to normality and then your experiences catch up with you. I sometimes struggle to sleep if I’m thinking about the unwell patients I’ve left in hospital, and I also worry about the patients who have survived intensive care and gone home. We have both been impacted by this crisis and need to focus on self-care going forward.'
If you are concerned about your mental health, see nhs.uk or ptsduk.org for more information and help
Olivia – who rebranded as Liv a few years ago – is a freelance digital writer at Marie Claire UK. She recently swapped guaranteed sunshine and a tax-free salary in Dubai for London’s constant cloud and overpriced public transport. During her time in the Middle East, Olivia worked for international titles including Cosmopolitan, HELLO! and Grazia. She transitioned from celebrity weekly magazine new! in London, where she worked as the publication’s Fitness & Food editor. Unsurprisingly, she likes fitness and food, and also enjoys hoarding beauty products and recycling.