’Tis the season to have (unprotected) sex
We’re more likely to engage in casual or unprotected sex during the festive period. But with STIs on the rise, you need to arm yourself against the main five
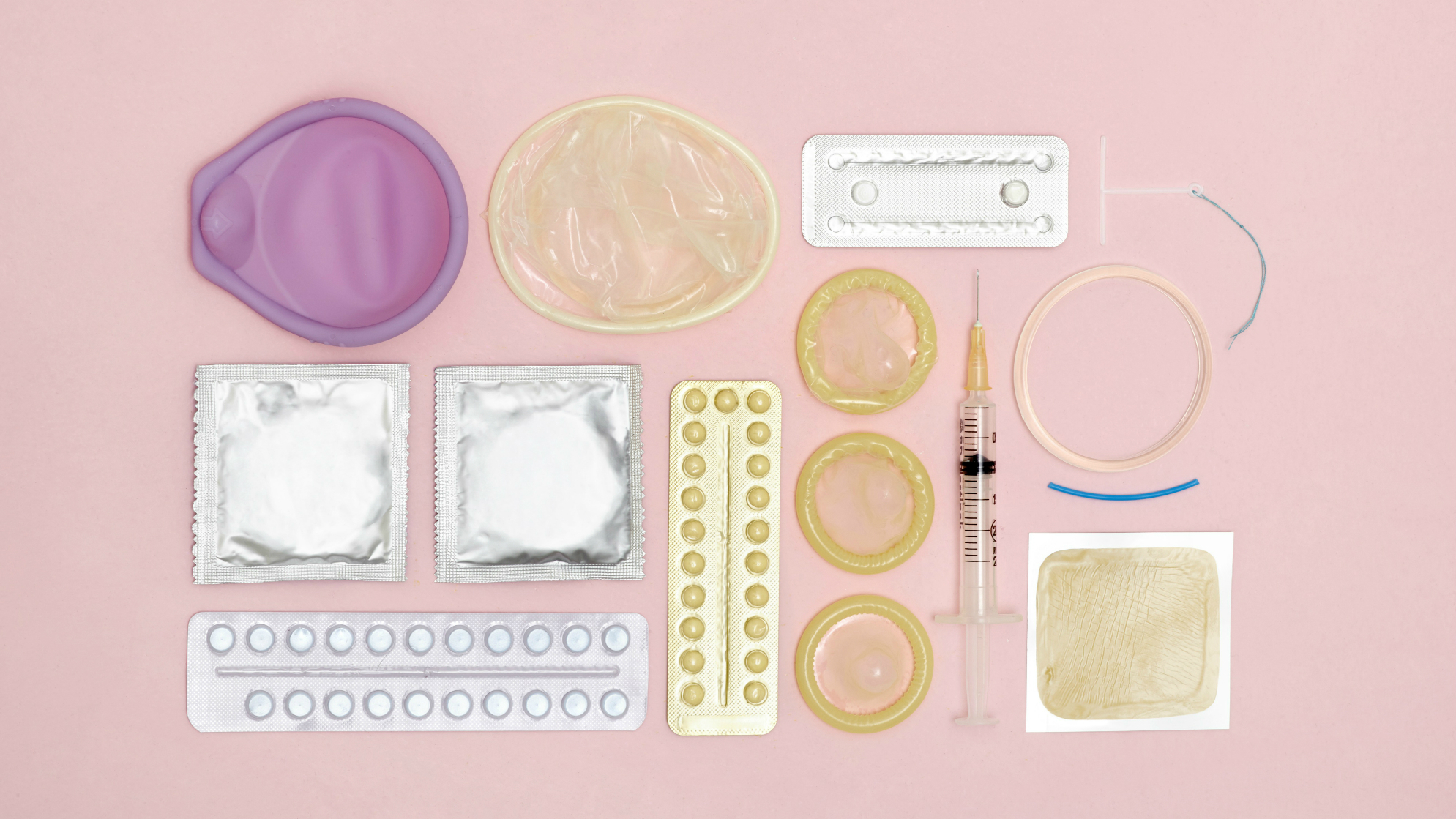
We’re more likely to engage in casual or unprotected sex during the festive period. But with STIs on the rise, you need to arm yourself against the main five
Words by Charlotte Haigh MacNeil
You might associate syphilis with Tudor monarchs, but according to a recent report by Public Health England, cases leapt up 76 per cent between 2012 and 2015. Meanwhile, gonorrhoea jumped up 13 per cent since 2017. And worryingly, the sexual-health charity FPA reveals that 68 per cent of Brits have never had an STI test, so could be unknowingly affected. This is bad news if you’re single and dating because several of the most common infections have serious long-term health consequences.
‘As the party season approaches, it’s a good time to evaluate your sexual health’, says Dr Claudia Estcourt, who specialises in sexual health. ‘People drink more at Christmas and it’s easier to get carried away and take risks. We see a rush in the clinic after the festive season as people have had unplanned sex and not used condoms so need an STI test or emergency contraception.’
Dating apps have also changed our sexual habits. ‘Women using apps like Tinder are having sex with more partners,’ says Estcourt. ‘In clinics, I’ve noticed they now talk about their sex lives with a new level of frankness.’
Her main three tips for the party season? Always use condoms with new partners. View a sexual health MOT as something you do regularly, like going to the dentist (if you’re having sex with new partners, aim for a check-up every three months). And once you get serious with a new partner, both book in for a full check-up before moving on to non-barrier methods like the Pill that do not protect you from STIs.
Here are the main five STIs to watch out for:
Chlamydia
What is it? The most common STI, with 220,000 cases a year in England alone, half of them in women. ‘The under-25 group is most affected but it’s far from exclusive – we see chlamydia in women through to their thirties,’ says Estcourt.
Celebrity news, beauty, fashion advice, and fascinating features, delivered straight to your inbox!
Symptoms: Bleeding after having sex and between periods, and pelvic or abdominal pain. However, 70 per cent of women don’t have any symptoms at all.
Risks: Pelvic inflammatory disease (PID), which can start when the bacteria progress through the cervix into the pelvis and can cause inflammation and scarring in the Fallopian tubes, leading to infertility and a raised risk of ectopic pregnancy.
How to treat it: Get a test – chlamydia can be treated simply with four antibiotic tablets you take all at once. ‘It’s also key to make sure your recent sexual partners are tested and treated if necessary, or you can be reinfected. Repeated chlamydia infections are more likely to lead to PID,’ says Estcourt. Use condoms to be safe.
HPV
What is it? The second-most common STI, the human papilloma virus (HPV) is actually a family of over 100 viruses, and some of them are responsible for genital warts.
Symptoms: Sometimes there are no symptoms at all, but if warts occur, they are small, fleshy growths that might crop up months after initial infection and can recur.
Risks: The strains of HPV that don’t cause warts have been linked with cervical cancer. ‘There’s also growing evidence of oral cancers being caused by certain types of HPV, which can be passed on during oral sex,’ says FPA chief executive Natika Halil.
How to treat it: Treatment usually involves using a topical cream to kill the warts, or they can be frozen or cut off. It’s passed on easily through skin-to-skin contact, so avoid sex if you or a partner has an active outbreak.

Genital herpes
What is it? Caused by the herpes simplex virus (HSV), this STI basically leads to cold sores down below.
Symptoms: ‘There are two strains,’ says Estcourt. ‘HSV1 usually causes cold sores around the mouth.’ About 70 per cent of us are affected, and if you’ve had cold sores in the past, you have some protection against contracting genital herpes through oral sex from someone with cold sores. HSV2, meanwhile, only causes genital herpes.
Risks: Just as with cold sores, genital herpes might crop up in the first two years after the initial infection, and often when you’re run-down.
How to treat it: Your doctor may prescribe acyclovir, which suppresses the virus and reduces symptoms or prevents flare-ups. Avoid sex if you or a partner has active herpes, and use condoms. ‘For oral sex, a dam (a square of plastic) can be used to form a barrier between the mouth and genitals,’ says Halil.
Gonorrhoea
What is it? The infection that used to be referred to as ‘the clap’, Public Health England figures show that gonorrhoea cases jumped by 13 per cent between 2017 and 2018.
Symptoms: It can cause a thick yellow or green discharge, pain when peeing and bleeding between periods, though half of women have no symptoms.
Risks: As with chlamydia, gonorrhoea can raise the risk of PID and infertility. It can be treated with antibiotics, but scientists are worried about a rise in cases of drug-resistant gonorrhoea.
How to treat it: It’s usually treated with an injection, then a tablet. Prevention is key – it’s passed in semen and vaginal fluids, so condoms will keep you safe.
HIV
What is it? The virus that can lead to AIDS. ‘HIV doesn’t affect large numbers of British women in their twenties and thirties,’ says Estcourt. ‘But all clinicians know someone who doesn’t fit the usual profile who has been affected, so you can’t afford to be complacent on this one.’
Symptoms: While some people have a mild illness when first infected, HIV usually has no symptoms until it starts to damage your immune system, often many years later.
Risks: HIV can be managed so most people with it can live long, healthy lives. But it’s still a serious condition that will affect your quality of life.
To treat it: Testing is important – if you’re HIV-positive, the sooner you start treatment, the better. Male or female condoms are the best way to prevent HIV, and use a lubricant designed for sex – this helps stop the small friction tears that can mean HIV is passed on more easily.
The leading destination for fashion, beauty, shopping and finger-on-the-pulse views on the latest issues. Marie Claire's travel content helps you delight in discovering new destinations around the globe, offering a unique – and sometimes unchartered – travel experience. From new hotel openings to the destinations tipped to take over our travel calendars, this iconic name has it covered.